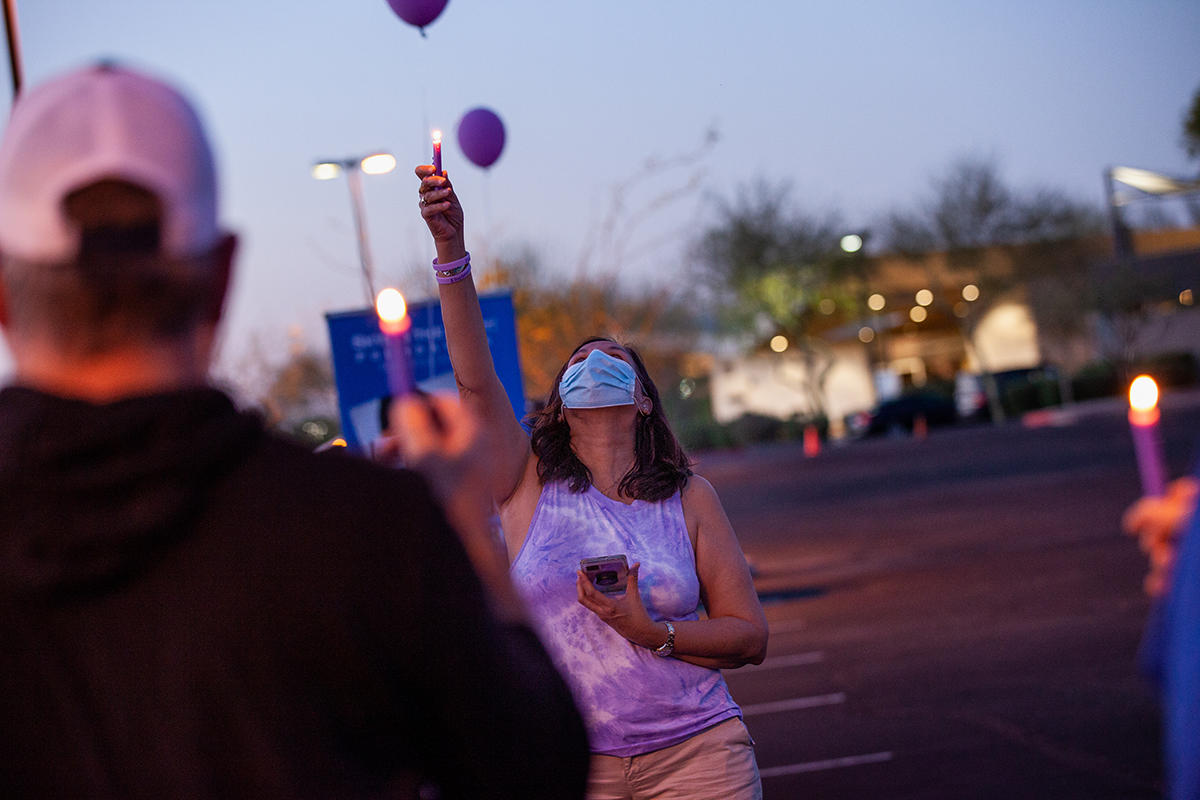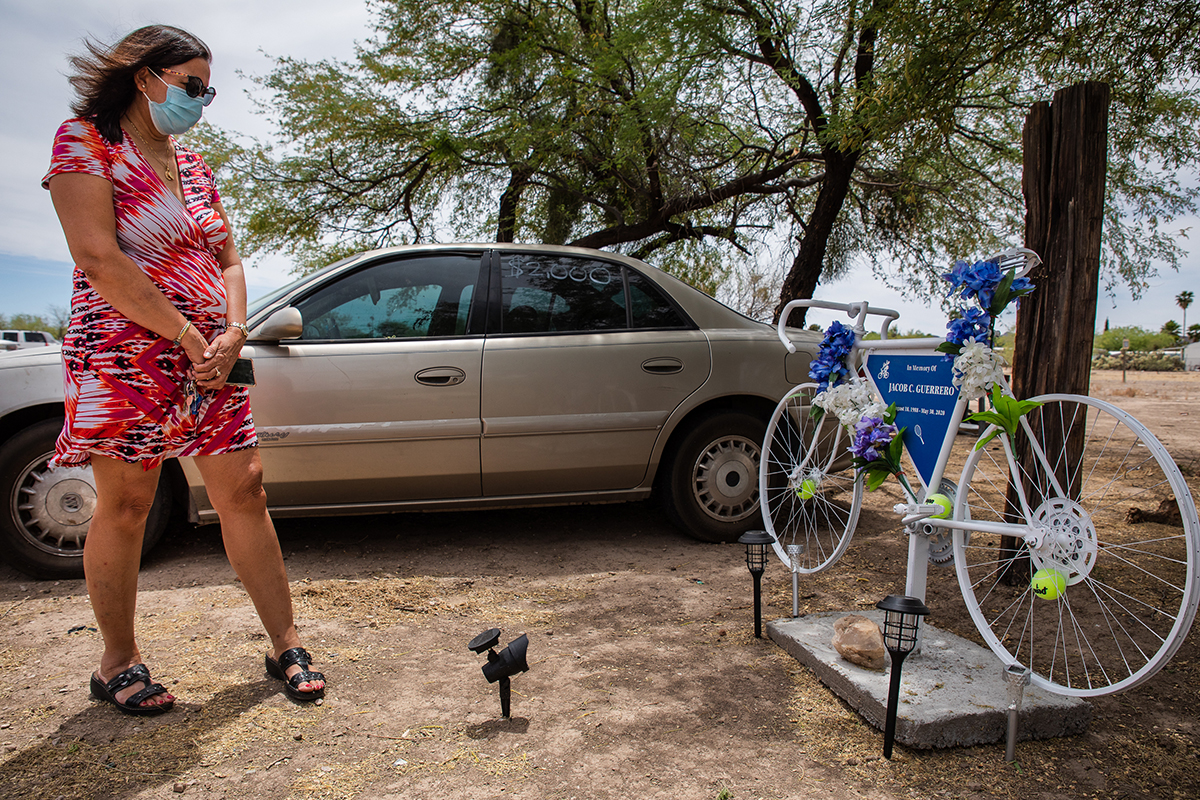TUCSON – It was a Tuesday afternoon, two months into the pandemic, when Theresa Guerrero got the call from her brother-in-law: Her son, Jacob, had been found unresponsive.
She was standing in the middle of a Ross store in south Tucson picking out a pillow he’d asked for, throwing it to the floor as she raced toward the exit.
Jacob was a cyclist, a tennis player – a trusting, good man – but he’d grown lethargic of late and quit pursuing his active lifestyle. The pandemic only made things worse.

A photo of Jacob Guerrero sits on a mantle dedicated to his memory inside Theresa Guerrero’s home in Tucson. Jacob, 31, died after using fentanyl-laced cocaine. (Photo by Alberto Mariani/Cronkite News)
He’d been working as a Postmates driver for a couple of months. One day, his mother saw straws in his car and wondered whether he was using cocaine. But when she confronted Jacob, he brushed her off.
“He was, like so many other people, really lonely, and I remember he would go on drives by himself just to get out of the house,” Guerrero said. “I have to wonder if he had been able to see other people, would they have noticed what he was going through before I did?”
By the time she drove the 7 miles to Jacob’s house last May 30, six paramedics were hovered over him. Guerrero doesn’t remember a lot about that moment, other than screaming out to strangers as they loaded her only son into an ambulance, assuming their silence meant the inevitable was coming.
She followed the lights and sirens to the hospital, but due to COVID-19 regulations, she had to stay outside and wait.
And wait.
“They finally let me in and directed me to sit down in a small room off to the side, and I instantly knew he was dead,” she said. “I couldn’t even call a priest in, so I prayed over him myself.”
At the age of 31, Jacob died of a fentanyl overdose. It was laced in cocaine he took that morning before a friend dropped him back home around 6 a.m. He was alive for about half the day, Guerrero thinks now – half a day to find and save him, wasted on a pillow she never bought.
An epidemic overshadowed
Long before former President Donald Trump declared a national emergency to fight the rapid spread of COVID-19, he declared the opioid crisis a public health emergency on Oct. 26, 2017. That year, more than 70,000 people died of an overdose – the majority involving opioids.
It was far from the worst the country would endure.
In the 12 months ending last September, at least 87,000 people died of a drug overdose in America, an increase of 27% from the previous 12 months and a record for the most such deaths in a single year, according to the Centers for Disease Control and Prevention.
Deaths attributed to synthetic opioids, mainly fentanyl, increased 53% nationwide in those same 12 months.
Increasingly, counterfeit prescription pills resembling oxycodone, Xanax and other medications – as well as illicit drugs, such as cocaine and heroin – are laced with fentanyl, a synthetic opioid 50 to 100 times more potent than morphine. Even 2 milligrams, the size of two grains of salt, can be fatal, according to the Drug Enforcement Administration.
In Arizona, preliminary numbers show 2,580 overdose deaths in the year ending last September, a 36% spike from the previous year. This means, on average, seven people in Arizona died every day from an overdose. Most of those deaths were due to synthetic opioids.
Although stay-at-home orders kept people safe from contracting COVID-19, home was where isolation, economic disruption and limited access to treatment fueled experimentation, and where experimentation led to addiction, relapse or death.
Support group meetings came to an abrupt halt, at least temporarily, and not everyone made the transition to telehealth. Outpatient treatment facilities lost track of patients.
“As we continue the fight to end this pandemic, it’s important to not lose sight of different groups being affected in other ways,” former CDC Director Robert Redfield said last December in a statement calling attention to the acceleration of overdose deaths. “We need to take care of people suffering from unintended consequences.”

Theresa Guerrero stands in the lot where her son overdosed last year. Guerrero was out shopping when she got the call that Jacob was unconscious. (Photo by Alberto Mariani/Cronkite News)
At the federal level, some steps have been taken to help.
Before the pandemic was declared in March 2020, federal law prohibited doctors from prescribing controlled substances without an in-person evaluation. That month, the DEA put the policy on hold for the duration of the pandemic, and specifically allowed doctors to prescribe medications to treat opioid addiction via the internet or telephone.
States also were granted the flexibility to allow opioid treatment programs to prescribe up to 28 days of take-home medication. Usually, patients on medication-assisted treatment are required to visit a facility daily to receive doses and counseling.
President Joe Biden is requesting $10.7 billion from Congress to support medication-assisted treatment, more research and additional behavioral health providers, with an emphasis on assisting Native Americans, older people and rural populations.
But more is needed to reverse the damage done during the pandemic, said Josephine Korchmaros, lead researcher for a University of Arizona program that aims to route people with opioid use disorders into treatment facilities instead of jail.
Even positive steps, such as more providers using telehealth to reach those with substance use disorders, come with roadblocks, Korchmaros said, noting that most of those she serves don’t have consistent access to phones and computers.
“Drug addiction has evolved with all of the additional stressors that come from the pandemic … and the stress and panic that come along with that,” she said.
“People cope with those feelings differently. Turning to substances is just one way.”
Dual crises prompt change
Since its founding in 1983, Scottsdale-based Community Medical Services has sought to help those struggling with drug addiction. Today, the company operates more than 40 clinics in nine states, including a 24/7 “opioid treatment on demand” center in Phoenix that serves about 300 people a day.
That clinic provides all three government-approved medications for opioid addiction treatment – buprenorphine, methadone and naltrexone – along with counseling and help with employment and housing.
During the pandemic, the clinic’s doors have stayed open, even if operations have a decidedly different look.
Before March 2020, patients would walk in and get evaluated, face-to-face, by a doctor. Those who were prescribed medication were required to report to the clinic daily to take it, and to participate in therapy sessions.
“We get them in right away, no questions asked,” said Jennifer Mason, vice president of operations, “because we know that the next time they use could be their very last.”
Since the beginning of the pandemic, the clinic’s mantra has been “minimizing contact, not care,” Mason said.
Now, patients are ushered into a room and evaluated using video chat on an iPad by a doctor one room over. Waiting room chairs are spaced out for social distancing, and clear shields have been added to the pickup windows where medications are distributed.
Before the pandemic, about 20% of patient interactions companywide were conducted online. By May 2020, that climbed to 88%, Mason said.

Community Medical Services staff members Kayleigh Lambert, left, and Lars Herrington talk about how the pandemic has affected drug prevention efforts. The 24/7 clinic in Phoenix provides medication-assisted treatment for those with opioid use disorder and has been using telehealth to reach patients. (Photo by Alberto Mariani/Cronkite News)
Kayleigh Lambert and other substance abuse counselors conduct virtual therapy sessions for an average of 20 to 25 people a day. Lambert has watched, in real time, as telehealth opened doors for people with social anxiety, parents who can’t afford a babysitter, or those not ready to step through the doors of a clinic to admit they have a problem.
“Clients don’t want to be in-person during COVID, and so if it’s the difference between ‘No, you have to come in or we can’t have a session’ and ‘No big deal, I’ll just call you on the phone later,’ it makes a lot more sense to extend that second invitation,” she said.
In addition to expanding telehealth, the clinic has been evaluating patients to make individualized decisions about take-home medication; most patients get a week’s worth at a time.
“If they don’t have their medication, they’re going to go to the emergency room, right? And that’s the last place that they need to go,” clinic manager Jesus Godinez said. “Let’s not overwhelm what is already an overwhelmed health care system.”
Because the approach reduces interactions with patients, a staff member makes periodic calls to check in.
“Sometimes we’re the only positive contact that our patients have, and to send them home, isolating them on the only days they used to come in, that’s not good,” Mason said. “There was no playbook for this, but we adapted the best we could.”
John Koch, director of community engagement for Community Medical Services, said that despite every advantage the online shift has granted the company, the stigma surrounding drug use continues to prevent people from seeking treatment, even in the privacy of their own homes.
More than any challenge the pandemic presented, stigma – the belief that people struggling with addiction lack the willpower to change, that drug use itself makes a person inherently bad — remains the toughest barrier to recovery, Koch said.
“Society,” he said, “has a really bad habit of trying to fit them into a box.”

Roberto Garcia distributes bags of supplies, including sanitation wipes and medication that can reverse opioid overdoses, to a group of homeless people outside Heritage Library in Yuma. Garcia, an outreach director at Sonoran Prevention Works, brings kits to the library once a week to try to prevent drug users from overdosing. (Photo by Alberto Mariani/Cronkite News)
‘Every loss is personal’
Once a week, Roberto Garcia meets a group at Heritage Library in Yuma to see how he can help those dealing with both substance use disorder and homelessness – and with how those problems have converged with the pandemic.
On this Saturday morning, five people are huddled under the shade of a willow tree as Garcia – a stout man with a dark, curly beard – approaches with a trash bag slung over his shoulder.
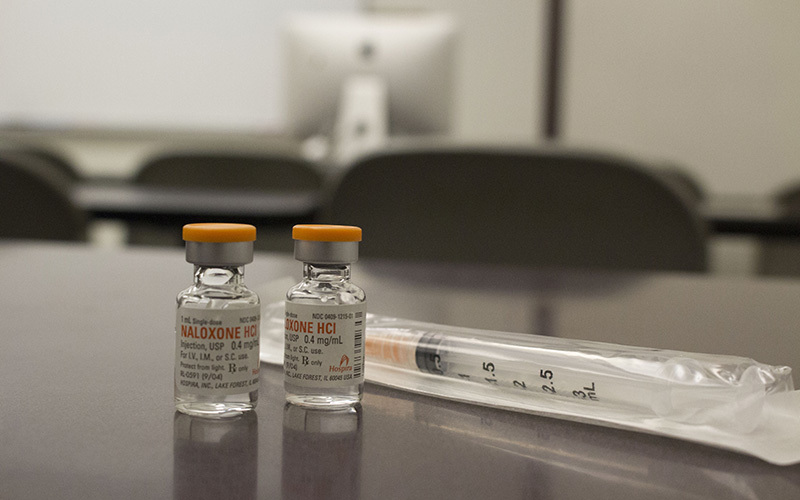
They call him Santa Claus, making Garcia laugh as he reaches a hand into his bag to grab body wipes and hand sanitizer, toothbrushes and toothpaste – and naloxone, more commonly known as Narcan, a medication designed to rapidly reverse opioid overdoses.
As he finally rests his back against the tree trunk, Garcia fields requests. Valery Jose, 50, asks for allergy medication – Garcia has that, too. Lonnie Patino wants cigarette lighters – Garcia pulls out a bag full of them in red, green, blue and yellow.
“Your choice – pass them around,” Garcia tells the group. He usually carries enough supplies for 20 people, the average crowd he met on the library lawn until this February, when police started forcing them out of public parks.
“They left them there the entire pandemic and then suddenly decided there were too many people in one space,” he said.

For three years, Garcia has worked as an outreach coordinator with Sonoran Prevention Works, an Arizona group that helps individuals and communities affected by drug use. A main goal is to help those still using do so more safely, by providing Narcan and test strips that can identify the presence of fentanyl in unregulated drugs.
Despite how much has changed this past year, Garcia’s world is largely the same. He still stops by the homes of patients but meets them outside. He added more hygiene products to his kits when public restrooms closed during the pandemic, leaving his homeless patients without a place to clean up.
Garcia, 34, has been in recovery himself for more than a decade. He was 4 when he had his first drink. By middle school, he was hooked on marijuana, prescription pills and then cocaine.
“I was raised in the same crisis I am now digging other people out of,” he said. “That’s how long Arizona has been in this.”
Garcia has a plan for this: “Meet people where they are at.” If someone wants to recover, he will be there to support them. But as long as they’re using, he will try to keep them alive.
Nowhere is his advocacy more important than in Yuma, he said. The city of roughly 96,000 is 185 miles southwest of Phoenix and sits near the Mexico border. Easy access to ports of entry promotes street trafficking “like you’ve never seen,” Garcia said.
Terry Wilson, one of the five gathered at the library, put it another way: “Towns like this, where everyone knows everyone, people think that sounds nice. But here it just means every loss is personal.
“It means you usually know the latest person you find in the gutter with a needle still stuck in their arm.”
Wilson, 29, started using fentanyl to manage back pain and never stopped. Like most of those sitting under the tree on this day, he has no intention of quitting.
Patino, 46, has struggled with addiction since he was 10, using methamphetamine, heroin and other substances. He doesn’t particularly enjoy or detest drugs – he sees using them as a matter of survival.
When he says this, the others nod in agreement.
“We’re not bad people,” Patino said. “We’re not good people, either. We’re neutral, which I think is the same thing as trying.”

Lonnie Patino sits in a park near Heritage Library in Yuma. Patino, who has struggled with addiction for over a decade, wants others to understand that drug users are not bad people. “We’re not good people, either,” he says. “We’re neutral, which I think is the same thing as trying.” (Photo by Alberto Mariani/Cronkite News)
‘Never say not my child’
Addiction forces a person to consider the fact that two things can be true at the same time: You can love your family and love drugs. You can value your career and value a high. You can make your own decisions and be incapable of making the one that just might save your life.
Theresa Guerrero understands all of this now. These days, wherever she goes, she carries Narcan nasal spray in her purse – as she has every day since Jacob died.
“You never know when someone might need it,” she said.
In March, Guerrero drove from Tucson to the Phoenix area to attend an event meant to bring renewed attention to the overdose epidemic. A purple trailer, traveling from Florida to Nevada, sat in the middle of a suburban church parking lot – with a picture of Jacob plastered on the back, next to the faces of dozens of others strung together by the common thread of tragedy.
Next to all the photos were messages: “Never say not my child.” “You never walk alone.” “See the goodness in all.”

After losing her son to a fentanyl overdose, Theresa Guerrero carries medication in her purse that can reverse opioid overdoses. “You never know when someone might need it,” she says. (Photo by Alberto Mariani/Cronkite News)
The annual event is organized by those who’ve lost loved ones to drugs. Before the pandemic, participants marched in the streets, but with COVID-19 restrictions varying from state to state, this year they elected to drive the trailer across America.
Lisa Maureen, who hosted the stop, lost her 20-year-old grandson, Demitri, to an overdose in 2018.
“It’s hard to grasp that the pandemic fueling this drug crisis is also preventing us from getting the word out about it,” she said. “We have done great work despite that, but it always feels like we could’ve done more, like we could’ve touched just one more person.”
Next to the trailer, tables held pamphlets, free masks, bottles of hand sanitizer – and a burlap blanket on which participants could write notes.
“I wish life would have been different for us,” one read. “If love could have saved you, you would have lived forever,” another said.